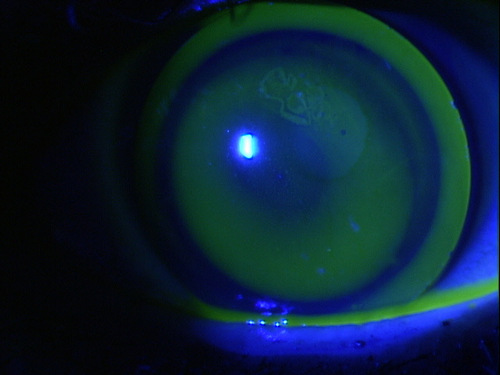
Corneal pachymetry maps showed mild thinning in the inferior part of the cornea of both eyes ( Fig. Examination of the corneal topography showed a marked protrusion of the paracentric inferior cornea in the right eye and a band-shaped, highly refractive area in the most peripheral part of the inferior cornea of the left eye ( Fig. 
There were no obvious abnormalities in the lens, vitreous cavity, and retina that could have caused the reduction of vision. She was aware of her unpleasant pruritus sensation that provoked her desire to rub her eyes. 
In addition, there were allergic changes in both conjunctivas with hyperemia and follicular formation in the upper eyelid. Slit-lamp microscopy showed an anterior protrusion of both corneas ( Fig. The intraocular pressure was 8 mmHg in the right eye and 17 mmHg in the left. We noted the very high astigmatism in both eyes. Her corrected decimal BCVA was 0.1 with a correction of −8.00 DS = −10.00 DC Ax 53° in the right eye and 1.0 with −0.50 DS = −7.00 DC Ax 103° in the left eye. There were no other relevant family histories. However, she reported that she had a history of atopic predisposition since her early childhood and had a habit of rubbing her eyes. After the age of 40 years, she had a decrease in her visual acuity in the right eye in spite of wearing the soft contact lenses, and she was referred to our hospital.Īt the initial examination, the patient had no specific complaints about the left eye. When she could no longer be corrected by conventional spectacles, she visited the eye clinic around the age of 30 years. The patient had been aware of the vision decrease in her right eye since she was about 20-years-old. We report our findings in this case and compare them with the findings of previous cases of PMCD and KC. We have examined a case of unilateral PMCD that progressed to a corneal perforation in a patient whose contralateral eye had KC. This may be because PMCD is much rarer than KC. The risk factor for acute hydrops in KC has been reported to be an atopic predisposition of the patient, 5 but there have been no reports describing the risk factors for acute hydrops in PMCD. The common denominator of both is that acute hydrops, a condition characterized by stromal edema due to leakage of aqueous into the stroma through a tear in Descemet's membrane, can develop when the corneal thinning is advanced causing the tears in Descemet's membrane. 4 The difference between the two disorders is that KC often occurs at a younger age, 10–20 years, while PMCD occurs after the age of 30 years. In addition, KC is often present in the contralateral eye of patients with PMCD. 3 The etiology of PMCD has not been definitively determined, but it is believed to be a disorder related to keratoconus (KC) because it is often seen in the same family. PMCD is more common in men than in women and is more often bilateral. Corneal analysis shows a “crab claw” pattern. This appearance has been described as a “beer belly” cornea. In these patients, slit-lamp microscopy shows a noninflammatory band of thinning in the periphery of the inferior cornea and an adjacent anterior protrusion of the upper region. 1 Patients often visit ophthalmologists in their 30s or later with a main complaint of vision decrease. Pellucid marginal corneal degeneration (PMCD), first described by Schlaeppi in 1957, is a relatively rare disorder that is associated with non-inflammatory thinning of the lower periphery of the cornea.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
